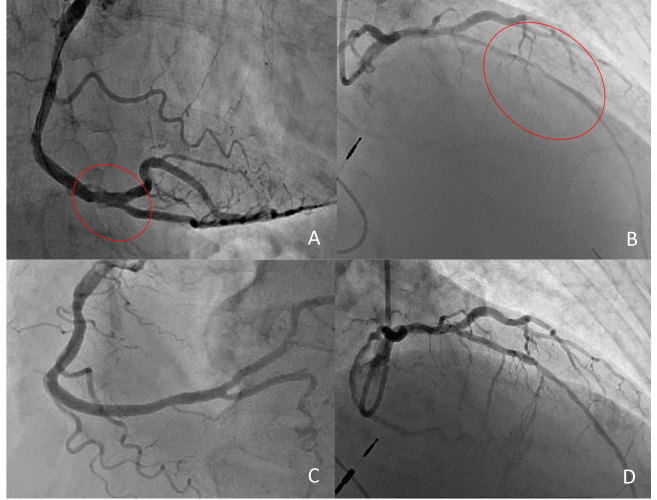
A few weeks ago, our study on DCB in native coronary vessels left with a dissection was published in JACC Int, and we had the honor of receiving a dedicated Editorial from 2 experts on the field: R Byrne and M Joner. Their conclusion was different from ours from several points of view, so we deemed necessary to underline further aspects and we wrote a Letter to the Editor.
The Letter was accepted for publication, and I am here anticipating it. I had the honor of sharing my ideas with F Alfonso.
Reply letter to: “Drug-Coated Balloon Angioplasty for De Novo Stenosis.
The Balloon is Back. Reloaded!”
Bernardo Cortese1, MD, and Fernando Alfonso2, MD
1 Interventional Cardiology, A.O. Fatebenefratelli, Milano, Italy
2 Interventional Cardiology, Hospital Universitario de La Princesa, Madrid, Spain
R. Byrne and M. Joner recently wrote an elegant editorial comment on a study that our group recently published in this Journal. (1, 2) We have to thank the two experts for their kind words regarding the importance of this type of proof of concept, independent studies. However, while reading the editorial we made several observations, that might be of some help for future discussions, and that we are going to summarize in the following points:
First, despite their enthusiasm for stents, Byrne and Joner should have also mentioned one of the major drawbacks of this technology, namely the risk of very late (and never ending) stent thrombosis. This concern has been shown to be a serious issue indeed both for first-generation and (at a lesser extent) second-generation drug-eluting stents.(3)
Second, we “enthusiastic adopters” of drug-coated balloons, would like to underline that this technology in not ‘against’ stents: on the contrary, it should be considered an adjunctive and complementary tool that should be available on the shelves of our cath labs. For example, but not exclusively, when you feel a stent is not the best choice: namely if the vessel is too small, when avoiding jailing a major side-branch appears reasonable, or if you already have several stent layers there as a result of recurrent in-stent restenosis.
Third, we concur that the results of our study should be considered as hypothesis-generating. However, some preclinical data also seem to confirm that paclitaxel, given at a single burst dose on the vessel wall, might facilitate vessel healing. (4, 5) Further studies will hopefully clarify this intriguing hypothesis.
Fourth, we fully agree with Drs Byrne and Joner that current guidelines still do not suggest drug-coated balloon use for native coronary vessels, but they should also mention that several expert consensus papers give clear indications for their use in this setting. (6, 7) We can only speculate on why the international guidelines do not reserve them a role in native vessels yet. Results of several currently ongoing clinical trials are eagerly awaited to definitively answer this important question.
In conclusion, we are well aware of the limitations of our study and we concur that stronger scientific evidence is required before a change in clinical practice may be recommended. However, we strongly believe that small, independent, well designed pilot studies are necessary to advance the field and draw the line for additional larger studies able to provide definitive clinical evidence.